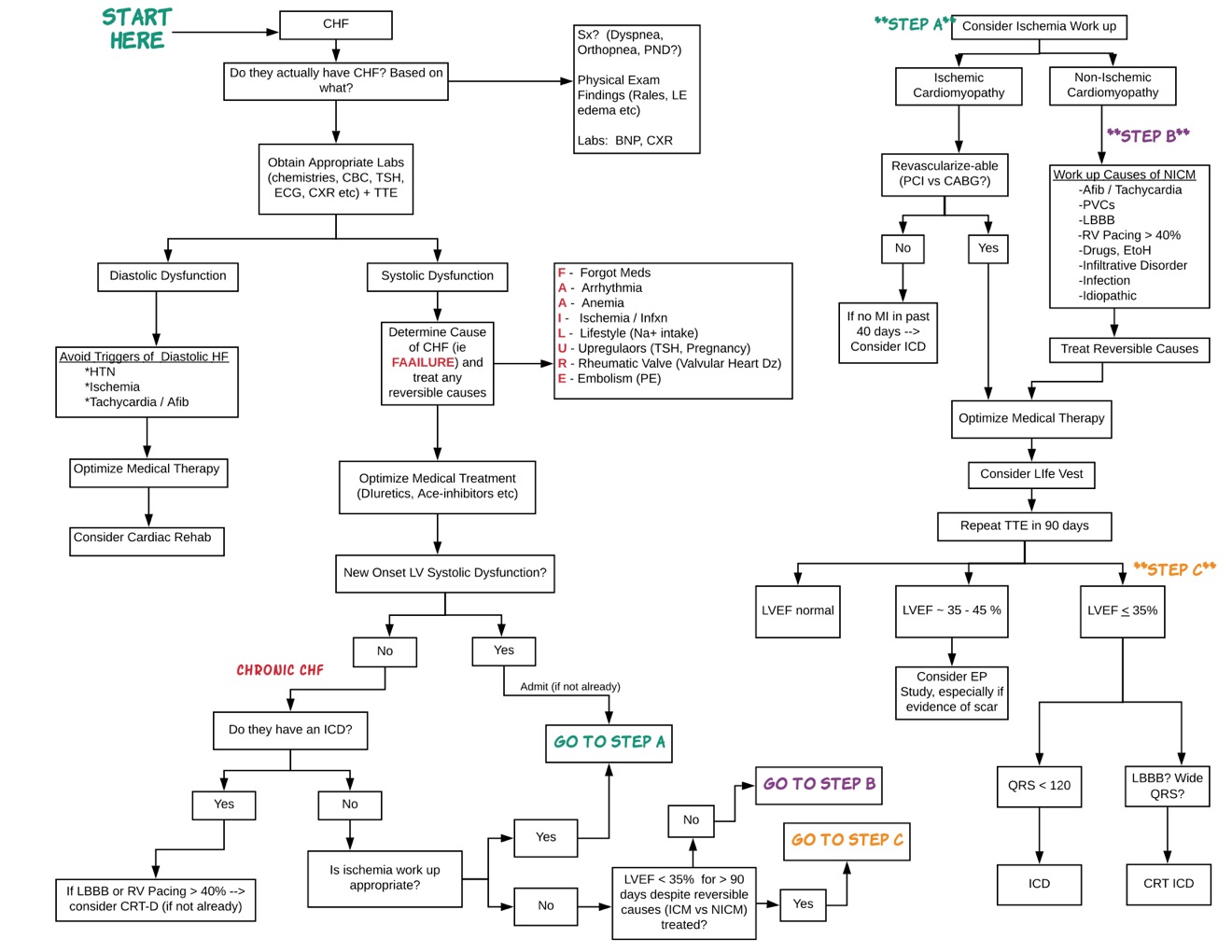
***SAMPLE CHF WORK SHEET***
HPI:
STEP ONE: Start by reviewing their cardiac history:
(a) Any History of CAD / MI / PCI / CABG?
-If so, list what symptoms they presented with (CP? SOB?) , what hospital they went to, what work did they have (TTE? Cath?)
(b) Any History of Afib:
-How did they present? How was it diagnosed?
-What symptoms do they have from Afib? (LH/dizziness, palpitations, racing heart rate sensation, syncope, pre-syncope, chest pain, dyspnea, fatigue, CHF etc)
-How were they treated? (Ever have a DCCV? Placed on any AAD or anticoagulation?)
(c) History of Pacemakers / ICD / CRT-D Device?
-What happened? How did they present? To what hospital?
(d) History of LBBB?
STEP TWO: List symptoms they presented with (Dyspnea, DOE, LE Edema, Orthopnea, PND, weight gain etc)
-How long have they had these symptoms?
-Chest pain? (substernal pressure / exertional / relieved with rest or NTG / duration of continuous pain)
STEP THREE: Determine ***WHY*** they went into CHF
F - Forgot Medications (non-compliance)
A - Arrhythmia
A - Anemia
I - Ischemia / Iron Overload / Infection
L - Life Style (increased Na+ intake = dietary indiscretions)
U - Upregulators (Thyroid Disease, Pregnancy)
R - Rheumatic Valve Disease (Valvular Heart Disease)
E - Emboli (Pulmonary Embolism)
ASSESSMENT & PLAN:
1. CHF (New onset / Acute on Chronic / Systolic / Diastolic / Combined systolic & diastolic Heart Failure)
(a) [Make an argument on why you think they have CHF]: The patient has CHF as evidenced by (list subjective findings + Physical Exam findings + Lab data)
Subjective Findings:
-Dyspnea / DOE
-Orthopnea
-PND
-LE Edema
-Weight Gain
Clinical Findings:
-JVD
-Rales
-Edema
Objective Findings:
-Elevated BNP
-CXR
-Cardiac Device information (if applicable)
***Please note that the Differential Diagnosis of Dyspnea is more than just “CHF” --> please make sure to have gone through a thorough consideration of the differential diagnosis of dyspnea. IE: if you make the argument that someone has a CHF exacerbation and they do NOT have subjective findings, clinical findings, or objective findings, have you really made a strong/compelling argument for CHF?”***
(b) [Insert Time line here] Putting their history of LV systolic dysfunction in relation to PCI, CABG, development of arrhythmias, pacing etc in a linear form is an incredibly powerful tool that can help you determine the cause of their LV systolic dysfunction (if they have it). Here is an example:
Baseline TTE: TTE 1.10.11: LVEF ~ 55-60%
Initial diagnosis of Afib: 3.1.12
Initial diagnosis of LV Systolic dysfunction: TTE 3.12.12: LVEF ~ 35% (while in a fib)
Coronary Angiography 3.18:12: No significant CAD
TEE-DCCV 3.19.12: AFib ----> normal sinus rhythm
TTE 5.25.12: LVEF ~ 55-60% (while in normal sinus rhythm)
ECG 8.16.17: Initial diagnosis of NEW LBBB
TTE 8.17.17: LVEF ~ 35% (while in normal sinus rhythm)
(c) [State here what you think the cause(s) of their CHF is]: Etiology of CHF exacerbation at this point is most likely: (go through FAAILURE and try to determine why they went into CHF). Please note that the time line you made above can be a great help with this step.
(c) [Put your treatment plan here]: Medical Therapy for this patient includes (List what CHF medications the patient is on, and if you want to change or make any additions to it). If the cause of CHF is reversible, you should make efforts to correct it.